Research-based and updated on September 24, 2021
If you haven’t yet read the first portion of this informational series, “What Happens to the Abdominal Muscles During a C-Section”, consider visiting that article first. That article shows that abdominal muscles do indeed get cut during a c-section. This article will show specific kind of cuts, usual practices & procedures of C-section, and videos in the operating room.
Historical Background
“The first documented cesarean delivery (CD) was in 1020 AD. In 1882, the era of modern CD began when Saenger advocated closing all uterine incisions immediately after surgery. The lower uterine segment incision was introduced by Kronig in 1912 and popularized in the United States by DeLee in 1922. The transverse uterine incision was described by Munro-Kerr in 1926…Approximately 2 CDs are started every minute in the United States alone; this is the most frequent major operation that is performed in this country.”1
Overview of the Tissues that Get Cut during a C-Section
How many layers are cut?!
Various references include various “numbers” of layers that are cut. Though this is a common web search query, it will not yield identical results every time because some layers of fascia are counted together in some references, while separated in other references. (For example, one could say – simplistically – that there are just 3 layers that are cut during a C-section: Skin, abdominal wall fascia, and then uterus. Some references use the number 7: skin, fat, fascia, muscles, more fascia, uterus, amniotic sac.2)
However many layers get cut, the reality is that, “to achieve a cesarean delivery, the surgeon must traverse all the layers that separate him/her from the fetus,”3 which absolutely include all fascia connected to the abdominal muscles. Here is one description that uses 4 layers.4
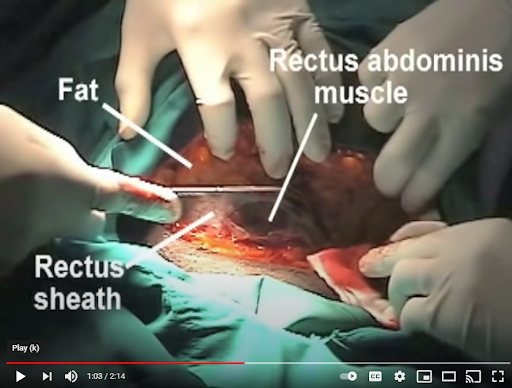
1. “First, the skin is incised, followed by the subcutaneous tissues.”
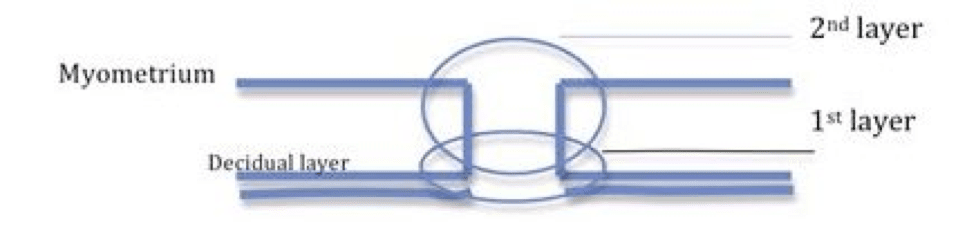
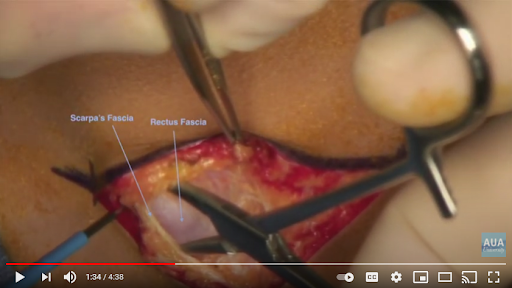
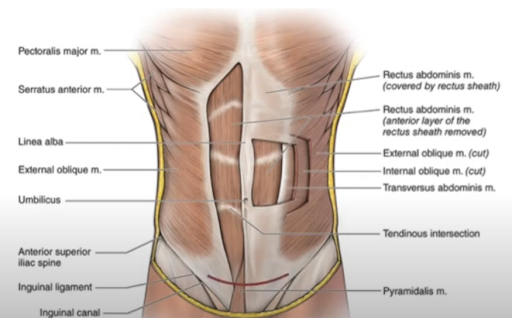
2. “The next layer is the fascia overlying the rectus abdominis muscles. The anterior abdominal fascia usually consists of two layers. One is composed of the aponeurosis from the external oblique rectus muscle, and the other is a fused layer which contains the aponeuroses of the transverse abdominis and internal oblique muscles.”
- Fascia – a thin sheath of fibrous tissue enclosing a muscle or other organ
- Aponeurosis – a sheet of fibrous tissue that takes the place of a tendon in flat muscles having a wide area of attachment
3. “After separating the rectus muscles…the surgeon enters the abdominal cavity through the parietal peritoneum.”
- Peritoneum – membrane lining the cavity of the abdomen and covering the abdominal organs
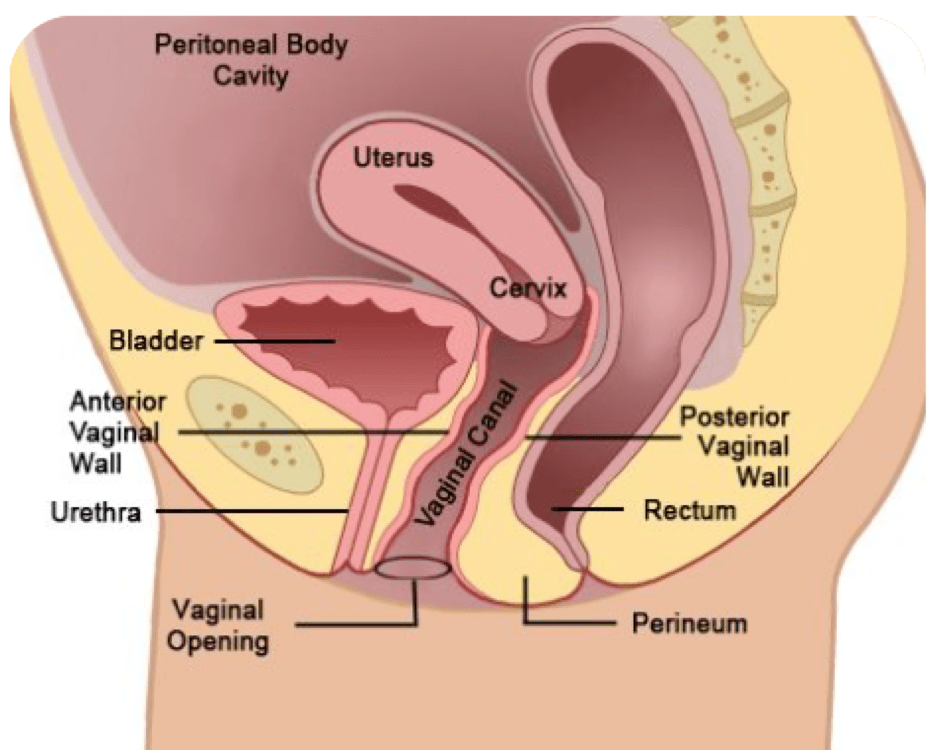
4. “Depending on the status of the patient’s amniotic membranes (if her “water is broken” or intact), the surgeon could encounter that amniotic sac upon incision of the uterus…The amniotic sac, if present, would be the last layer between the surgeon and the fetus. It is at this point that the fetus is delivered, achieving the primary goal of the cesarean section.”
According to 2010 research in Gynecological Surgery, “At the most basic level, the only thing necessary is some cutting instrument. In an emergency, a physician could theoretically perform a perimortem cesarean delivery on a woman after a car accident with a sharp piece of glass.”5 Equipment used can include: catheter running from the bladder, regional or general anesthesia, and a surgical tray that includes scissors, bandages, clamps, forceps, retractors, needle drivers and more.
The four main cesarean delivery techniques are6:
- Pfannenstiel-Kerr – Pfannenstiel skin incision, followed by multiple sharp dissections (not blunt), closure of peritoneum, interrupted fascia closure, continuous skin suture.
- Joel-Cohen – JC skin incision, followed by multiple blunt dissections, spontaneous placenta removal, non-closure of peritoneum
- Misgav-Ladach – Same as JC (JC skin incision and blunt dissections), except: Misgav-Ladach uses manual placenta removal (not spontaneous), single layer running closure of the uterus (not interrupted), continuous closure of the fascia (not interrupted), mattress closure of the skin (not continuous)
- Modified Misgav-Ladach – Pfannenstiel skin incision, followed by multiple blunt dissections, spontaneous placental removal, running uterine closure (not interrupted), closure of the peritoneum, continuous closure fascia closure, continuous skin suture.
Explanation of Closure/Sutures:
- Continuous/Running = single thread
- Interrupted = multiple small threads, one after the other
- Berghella, et al. Evidence-based surgery for cesarean delivery. American Journal of Obstetrics & Gynecology. Retrieved 4/21/21 from https://www.ajog.org/article/S0002-9378(05)00500-4/fulltext ↩︎
- [n.d.] You’ve had a C-section – now what? Carolina Pelvic Health Center, Inc. Retrieved 9/24/24 from https://carolinapelvichealth.com/c-section-birth-your-guide-to-recovery/#:~:text=A%20C%2Dsection%20includes%207,and%20finally%20the%20amniotic%20sac. ↩︎
- 2023. Sung, Sharon. Mahdy, Heba. Cesarean Section. StatPearls [Internet]. Retrieved 8/21/24 from https://www.ncbi.nlm.nih.gov/books/NBK546707/ ↩︎
- 2023. Sung, Sharon. Mahdy, Heba. Cesarean Section. StatPearls [Internet]. Retrieved 8/21/24 from https://www.ncbi.nlm.nih.gov/books/NBK546707/ ↩︎
- 2023. Sung, Sharon. Mahdy, Heba. Cesarean Section. StatPearls [Internet]. Retrieved 8/21/24 from https://www.ncbi.nlm.nih.gov/books/NBK546707/ ↩︎
- 2023. Sung, Sharon. Mahdy, Heba. Cesarean Section. StatPearls [Internet]. Retrieved 8/21/24 from https://www.ncbi.nlm.nih.gov/books/NBK546707/ ↩︎
- 2023. Sung, Sharon. Mahdy, Heba. Cesarean Section. StatPearls [Internet]. Retrieved 8/21/24 from https://www.ncbi.nlm.nih.gov/books/NBK546707/ ↩︎
- 2010. Bolla, et al. Technical aspects of the cesarean section. Gynecological Surgery. Retrieved 4/21/21 from https://gynecolsurg.springeropen.com/articles/10.1007/s10397-010-0560-9 ↩︎
- 2010. Bolla, et al. Technical aspects of the cesarean section. Gynecological Surgery. Retrieved 4/21/21 from https://gynecolsurg.springeropen.com/articles/10.1007/s10397-010-0560-9 ↩︎
- 2010. Bolla, et al. Technical aspects of the cesarean section. Gynecological Surgery. Retrieved 4/21/21 from https://gynecolsurg.springeropen.com/articles/10.1007/s10397-010-0560-9 ↩︎
- 2015. Gizzo, et al. Caesarean Section: Could Different Transverse Abdominal Incision Techniques Influence Postpartum Pain and Subsequent Quality of Life? A Systematic Review. PLOS ONE. Retrieved 4/21/21 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4315586/ ↩︎
- 2010. Bolla, et al. Technical aspects of the cesarean section. Gynecological Surgery. Retrieved 4/21/21 from https://gynecolsurg.springeropen.com/articles/10.1007/s10397-010-0560-9
↩︎ - 2023. Sung, Sharon. Mahdy, Heba. Cesarean Section. StatPearls [Internet]. Retrieved 8/21/24 from https://www.ncbi.nlm.nih.gov/books/NBK546707/ ↩︎
- 2016. Cesarean Section/Cesarean Delivery. Stepwards. Retrieved 4/21/21 from https://www.stepwards.com/?page_id=3610 ↩︎
- 2016. Cesarean Section/Cesarean Delivery. Stepwards. Retrieved 4/21/21 from https://www.stepwards.com/?page_id=3610 ↩︎
- 2016. Cesarean Section/Cesarean Delivery. Stepwards. Retrieved 4/21/21 from https://www.stepwards.com/?page_id=3610 ↩︎
- 2010. Bolla, et al. Technical aspects of the cesarean section. Gynecological Surgery. Retrieved 4/21/21 from https://gynecolsurg.springeropen.com/articles/10.1007/s10397-010-0560-9 ↩︎
- 2020. AUAUniversity. Core Videos (2019): Open Surgical Approaches: Pfannenstiel Incision. YouTube. Retrieved 4/21/21 from https://www.youtube.com/watch?v=Yma-72HE0NA ↩︎
- 2021. Melbourne Uni Radiology Masters. Retropubic Space. Radiopaedia. Retrieved 9/24/21 from https://radiopaedia.org/articles/retropubic-space?lang=us#:~:text=The%20retropubic%20space%20(also%20known,the%20level%20of%20the%20umbilicus. ↩︎
- [n.d.] Micheau, Antoine. Extraperitoneal space. e-Anatomy at IMAIOS. Retrieved 9/24/24 from https://www.imaios.com/en/e-Anatomy/Anatomical-Parts/Extraperitoneal-space#:~:text=The%20extraperitoneal%20space%20is%20the,situated%20posteriorly%20to%20the%20peritoneum ↩︎
- 2024. O’Neill, Katie. The Peritoneum. TeachMeAnatomy. Retrieved 9/24/24 from https://teachmeanatomy.info/abdomen/areas/peritoneum/#:~:text=The%20peritoneum%20is%20a%20continuous,to%20and%20from%20the%20viscera.
↩︎ - [n.d.] Micheau, Antoine. Extraperitoneal space. e-Anatomy at IMAIOS. Retrieved 9/24/24 from https://www.imaios.com/en/e-Anatomy/Anatomical-Parts/Extraperitoneal-space ↩︎
- 2019. AUAUniversity. Core Videos (2019): Open Surgical Approaches: Pfannenstiel Incision. YouTube. Retrieved 8/21/21 from https://www.youtube.com/watch?v=Yma-72HE0NA ↩︎
- [n.d.] Rectus Sheath. Wikipedia. Retrieved 4/21/21 from https://en.wikipedia.org/wiki/Rectus_sheath ↩︎
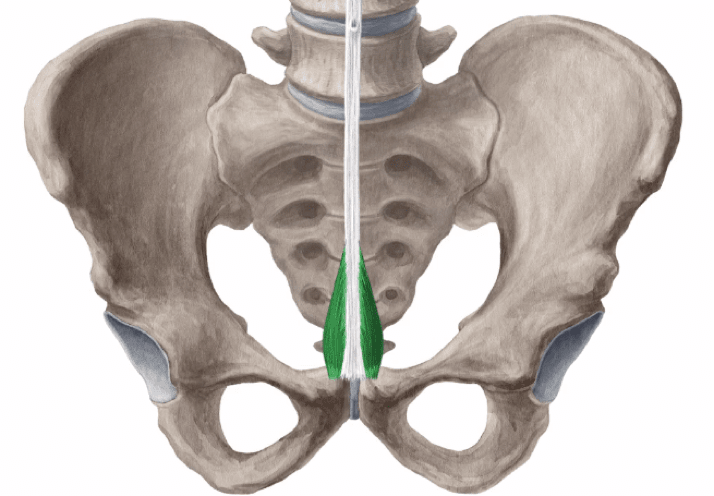
- 2023. Vaskovic, Jana, MD. McLaren, Nicola, MSc. Pyramidalis muscle. KenHub. Retrieved 4/21/21 from https://www.kenhub.com/en/library/anatomy/pyramidalis-muscle
↩︎ - 2020. Hojaij, et al. Morphometry and Frequency of the Pyramidalis Muscle in Adult Humans: A Pyramidalis Muscle’s Anatomical Analysis. Clinics. Retrieved 4/21/21 from https://www.scielo.br/pdf/clin/v75/1807-5932-clin-75-e1623.pdf
↩︎ - 2017. Swaroop Das, et al. Biometrics of Pyramidalis Muscle and its Clinical Importance. Journal of Clinical & Diagnostic Research. Retrieved 4/21/21 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5376864/#:~:text=Pyramidalis%20is%20classified%20as%20a,and%20in%20various%20surgical%20procedures. ↩︎
- 2017. Swaroop Das, et al. Biometrics of Pyramidalis Muscle and its Clinical Importance. Journal of Clinical & Diagnostic Research. Retrieved 4/21/21 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5376864/#:~:text=Pyramidalis%20is%20classified%20as%20a,and%20in%20various%20surgical%20procedures. ↩︎
- Image: 2023. Vaskovic, Jana, MD. McLaren, Nicola, MSc. Pyramidalis muscle. KenHub. Retrieved 4/21/21 from https://www.kenhub.com/en/library/anatomy/pyramidalis-muscle
↩︎ - 2017. Swaroop Das, et al. Biometrics of Pyramidalis Muscle and its Clinical Importance. Journal of Clinical & Diagnostic Research. Retrieved 4/21/21 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5376864/#:~:text=Pyramidalis%20is%20classified%20as%20a,and%20in%20various%20surgical%20procedures.
↩︎ - 2015. Natsis, et al. Morphometric variability of pyramidalis muscle and its clinical significance. Surgical and Radiologic Anatomy. Springer Link. Retrieved 9/24/24 from https://link.springer.com/article/10.1007/s00276-015-1550-4
↩︎ - 2020. Hojaij, et al. Morphometry and Frequency of the Pyramidalis Muscle in Adult Humans: A Pyramidalis Muscle’s Anatomical Analysis. Clinics. Retrieved 4/21/21 from https://www.scielo.br/pdf/clin/v75/1807-5932-clin-75-e1623.pdf
↩︎ - [n.d.] Transversalis fascia. e-Anatomy at IMAIOS. Retrieved 9/24/24 from https://www.imaios.com/en/e-Anatomy/Anatomical-Parts/Transversalis-fascia ↩︎
- [n.d.] Transverse abdominal muscle. Wikipedia. Retrieved 9/24/24 from https://en.wikipedia.org/wiki/Transverse_abdominal_muscle ↩︎
- 2023. Yu, Yoshi. Arcuate Line. Radiopaedia. Retrieved 9/24/24 from https://radiopaedia.org/articles/arcuate-line?lang=us ↩︎
- 2013. Openmichigan. Caesarean Section: Step 2 – Abdominal Incision. YouTube. Retrieved 9/24/24 from https://www.youtube.com/watch?v=lMQLE7Ruk0Q ↩︎
- 2010. Drkapilkishore. Cesarean birth / C Section / LSCS/ Child Birth. YouTube. Retrieved 9/24/24 from https://www.youtube.com/watch?v=gJeRWGxOTcA ↩︎
- 2020. Dr Rahul Jadhao. Misgav Ladach technique of caesarean section -Dr Rahul Jadhao. YouTube. Retrieved 9/24/24 from https://www.youtube.com/watch?v=U8lARiRmV3E ↩︎
- 2012. Hammydude12345. Cesarean Section Operative Technique. YouTube. Retrieved 9/24/24 from https://www.youtube.com/watch?v=dwlwREGR8sM ↩︎